Vasectomy
Northampton Medical Services Ltd offer you the latest and more advanced technique by performing a no-scalpel vasectomy. Both of our doctors are members of BANSV (British Association of No-Scalpel vasectomists) and ASPC (Association of Surgeons in Primary Care). This procedure does not use a scalpel to make a cut in each side of the scrotum. Instead only one small keyhole is made under local anaesthetic in the mid-line and the vas (sperm tube) from each side are lifted through this. A small section of the vas is removed, the ends are cauterised and then placed back into the scrotum.
This scalpel-free method is an advanced technique, not yet widely available (most hospitals tend to use the old scalpel technique). The advantages of the no-scalpel vasectomy compared with the traditional scalpel method are:
* Less pain
* No stitches
* Less damage to the tissues
* Shorter operating time
* Faster recovery
* Reduced complications like bleeding & haematoma formation (clot in the scrotum)
* Reduced risk of infection
What happens during a vasectomy?
The vas is the medical name for the tube along which the sperm travel from the testes to the penis. During vasectomy procedure approximately 5mm is removed from each vas and the ends are cauterised. This prevents the sperm from joining the semen at ejaculation. The operation can be carried out under local anaesthetic and this is obviously a safer way of doing it. There is a small amount of discomfort for a matter of seconds while the anaesthetic is infiltrated into the skin of the scrotum and around the sperm tubes (it feels similar to having local anaesthetic prior to having a tooth filled). In fact the discomfort associated with a vasectomy may be compared to having a tooth filled, both in terms of the procedure, the anaesthetic and the post-op discomfort. Rarely if the vas are difficult to feel, it may not be possible to do the operation under local anaesthetic and a general anaesthetic would be required, this will be decided during assessment prior to the procedure.
How effective is a vasectomy?
Vasectomy must be considered a permanent form of contraception. It remains the most effective form of male contraception, however, there is a very small failure rate where the two ends of the tube grow together again. This happens in about 1 in 2000 cases over the rest of the man's lifetime.
Will a vasectomy affect my ability to have sex?
The operation does not affect the ability of the man to perform sexual intercourse and does not affect sexual drive in any way. Seminal fluid will continue to be ejaculated when a man reaches a climax but it will not contain sperm. The testicles continue to produce the hormone, testosterone, which is responsible for masculine qualities. In other words, the operation does not affect a man's sexuality.
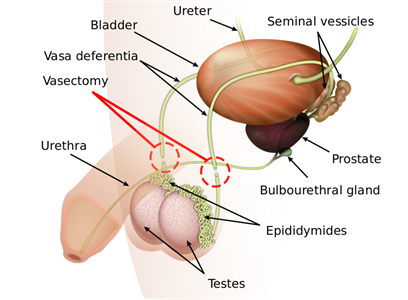
Before the Operation:
Please ensure that the scrotum ("the bag" holding the testes) is free of hair. It may mean having to shave the scrotum (below the penis). You can use a safety razor to clip the hair. It helps to reduce the incidence of infection and makes the operation technically convenient. Please do this a day before or on the day of the operation.
Also bring a pair of tight-fitting underpants, if available, to wear after the operation. Postoperatively, it provides extra support.
What happens after the operation?
- Some minimal bruising and discomfort may be expected during the first 1-3 days and this may resolve without treatment, although it is usual to take something for this discomfort such as Paracetamol or Ibuprofen. The small puncture wound on your scrotum is likely to ooze a little for the first few days and then scab over. Sometimes a drop or two of blood might stain the first couple of ejaculations after the procedure which is due to congestion at the cut end of the tube.
- After the operation, the remainder of the day should be spent resting, as well as the following 2 days. We advise you to wear tight fitting underpants to support your scrotum day and night for 1 week. It is important to avoid heavy lifting, heavy physical work, vigorous exercise, sport and intercourse for at least one week. Depending on the patient's occupation, it may be necessary to take up to one week off work. This is not a reflection on the severity of the operation, rather that the scrotum is very mobile and subject to friction and needs rest to allow all tissues to seal and heal. REST IS IMPORTANT FOR THE FIRST 24-48 HOURS. IF THIS ADVICE IS IGNORED COMPLICATIONS SUCH AS BLEEDING, INFECTION, PAIN AND SWELLING ARE MORE COMMON.
When will a vasectomy be effective?
It is essential that the couple must use other forms of contraception following the vasectomy operation until the man has had at least one sample of semen examined to make sure that there are no sperm present. It is advised to have a minimum of 30-40 ejaculations before sending the sample to the laboratory at 16 weeks after the operation. In a small number of cases the test will not be fully clear and the test will have to be repeated. Very occasionally the semen may be very slow to clear and sperm can be present more than a year after the operation. Once we have a semen test that shows no sperm present we will write to you to advise that you are sterile. Under certain circumstances the production of small numbers of dead sperm can be acceptable and 'special clearance' can be given, however the dcotor would discuss and advise on this if appropriate.
What are the possible complications?
- Surgical wound infections (1%) occur from time to time and the puncture wound may be slow to heal. This may need to be re-checked by the doctor in case it requires antibiotic.
- Scrotal haematoma (blood clot) occurs in about (1-2%) of cases. Some bleeding into the tissues around the testicle causes it and gives rise to pain and swelling. This is commonest during the first 2-3 days, is likely to occur if stipulation regarding rest is not observed and could take few weeks to resolve.
- Epididymitis or Epididymo/Orchitis occurs in about 0.5% and is a condition in which part or the entire testicle becomes inflamed. This can occur following a vasectomy. It can also occur in men who have not had a vasectomy. It is rare and usually responds well to treatment.
- Sperm Granuloma may occur in up to 1% of vasectomy cases. These are small lumps, which form at the end of the vas, particularly on the side still carrying sperm. These are harmless and usually do not cause any problems but if they become tender or painful it may be necessary to remove them surgically. This procedure can be done under local anaesthetic.
- Rarely men suffer from persistent pain in the testicle or at the vasectomy site which does not have an obvious cause and occurs in 1 man in every 300-400 vasectomies. This is called 'post vasectomy pain syndrome'. Treatment of this condition is sometimes difficult, in some of the cases it subsides with time and on rare occasion might require reversal of the procedure.
Should you have any further question to ask, please contact your doctor at your surgery, or contact Northampton Medical Services using the contact form on this website


